The detection of SARS-CoV-2 is based on the identification of viral RNA from respiratory samples by RT-PCR. Currently, the standard method for the detection of SARS-CoV-2 infection is the one that includes the nasopharyngeal swab, but there are other alternatives (nasal swab, oropharyngeal swab or saliva) whose sensitivity and specificity are under discussion.
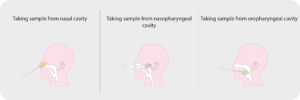
Figure 1. Differences between nasal swab, nasopharyngeal swab and oropharyngeal swab.
However, the use of nasopharyngeal swab has certain drawbacks, such as the need for a large number of specialized personnel and, often, shortage of swabs, which translates into a greater economic and logistical burden for health system. It also represents a risk of viral transmission for the person who takes the sample. Responding to the need to find a simpler and less invasive method, saliva emerges as a candidate for sample collection. The use of saliva for the diagnosis of SARS-CoV-2 has several advantages: the simplicity of the collection of the sample, the reduction of the risk of virus transmission to healthcare staff and the least discomfort for the patient. The use of alternative samples to the nasopharyngeal swab opens the debate on the reliability and sensitivity of the saliva sample for the diagnosis of SARS-CoV-2.
In general, saliva tests appear to have lower sensitivity compared to the use of nasopharyngeal swab. A study published in Infectious Diseases Society of America shows a lower sensitivity in detecting the virus using saliva as a sample. Specifically, nasopharyngeal swabs were 17% more sensitive than saliva in the number of detectable positives. In addition, a greater difference in sensitivity was observed between both methods of sample collection, especially if the individual fell ill later on, so that the difference in sensitivity was 6% in samples collected during the first days of the disease and the 20% in samples collected from the second week of the disease.
Therefore, to date, there is not enough evidence to consider saliva as a valid option to nasopharyngeal swab for the detection of the virus. Although nasal swab, which is more comfortable for the patient, has been found to have a sensitivity comparable to the nasopharyngeal swab, thus being able to be used as a reliable alternative to the standard method of disease diagnosis caused by the SARS-CoV-2 virus.





